Heterophile antibodies are produced in response to antigens produced during EBV IM (EBV heterophile antigens or Paul–Bunnell antigens) or as a result of serum sickness (type III hypersensitivity reaction caused by proteins present in certain medications) or rheumatoid factors (non-EBV heterophile antigens or Forssman …
What are heterophile antibodies and how do they relate to EBV?
In clinical diagnosis, the heterophile antibody test specifically refers to a rapid test for antibodies produced against the Epstein-Barr virus (EBV), the causative agent of infectious mononucleosis. Heterophile antibodies can cause significant interference in any immunoassay.
What are heterophile antibodies and how are they formed?
Heterophile antibodies are antibodies produced against poorly defined antigens. These are generally weak antibodies with multispecific activities. Human anti-animal antibodies that develop as a result of treatments with animal immunoglobulins are antibodies with strong avidities, produced against well-defined antigens.
What are heterophile antibodies in EBV?
The heterophile antibody is an immunoglobulin M (IgM) antibody produced by infected B lymphocytes. It is not directed against Epstein-Barr virus (EBV) or EBV-infected cells, but it is a result of the infection and the subsequent transformation of the B cell to a plasmacytoid state.What does a heterophile antibody do?
Heterophile antibodies are endogenous antibodies in human serum/plasma that may interfere with immunoassays resulting in false elevation, or rarely false depression of measured values.
What causes the body to produce antibodies?
The immune system cells produce antibodies when they react with foreign protein antigens, such as infectious organisms, toxins and pollen. At any given time, the body has a large surplus of antibodies, including specific antibodies that target thousands of different antigens.
Which antibody is more specific for infectious mono heterophile AB or EBV AB?
Since heterophile antibodies typically return quicker than EBV specific antibodies, it is the test of choice in most clinical settings to determine if an individual has infectious mononucleosis.
What is heterophile specificity?
Heterophile antibodies are low-affinity IgM antibodies with broad specificity for predominantly carbohydrate antigens that can react with molecules found on the surface of a number of nonhuman erythrocytes (hence heterophile = other loving).What particles can Heterophile antibody Agglutinate?
Heterophile antibodies are IgM antibodies, which agglutinate erythrocytes from different species including bovine, camel, horse, goat, and sheep.
How do you test for Heterophilic antibodies?Process. The test is usually performed using commercially available test kits which detect the reaction of heterophile antibodies in a person’s blood sample with horse or cow red blood cell antigens. These test kits work on the principles of latex agglutination or immunochromatography.
Article first time published onWhat is Paul Bunnell test used for?
The Paul Bunnell test is used to screen for Infectious Mononucleosis (IM), which is seen most commonly in adolescents and young adults. IM is caused by the Epstein-Barr virus.
What cell population is typically infected by EBV?
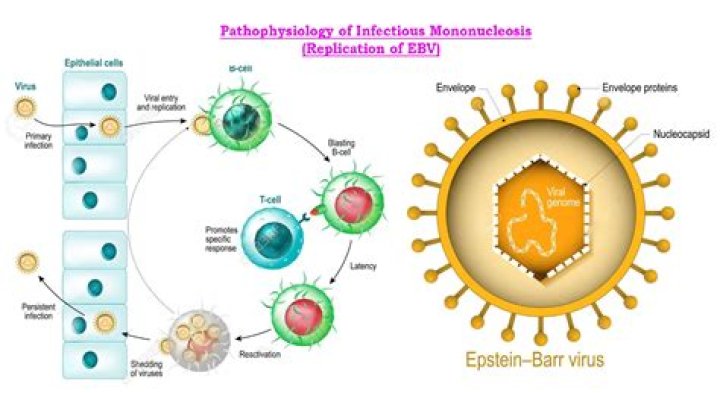
In healthy hosts, B lymphocytes and epithelial cells are the cellular targets for EBV primary infection. However, the EBV can infect a wide range of non-B lymphocytes, and it critically affects the development and pathogenesis of EBV-related diseases (63).
How autoantibodies are formed?
(A) Autoantibodies produced by B lymphocytes bind to self-antigens released by apoptotic or necrotic cells, forming antigen–antibody (immune) complexes. When antigens in the immune complexes contain nucleic acids and are endocytosed by pDCs, Toll-like receptors are activated and the pDCs secrete interferon-α.
What is hook effect in Elisa?
The hook effect happens when there is an excessive amount of analyte in one-step immunoassay. … Where there is an excessive amount of analyte, they overwhelm the capture antibody; this allows the excess analyte to bind to the detection antibody directly, hence preventing the formation of the antigen-antibody sandwich.
How are monoclonal antibody drugs made?
A monoclonal antibody is created by exposing a white blood cell to a particular viral protein, which is then cloned to mass produce antibodies to target that virus. Prior to COVID-19, monoclonal antibodies were developed to treat several viral infections, such as Ebola and rabies.
What is EBV antibody profile?
Presence of VCA IgM antibodies indicates recent primary infection with Epstein-Barr virus (EBV). The presence of VCA IgG antibodies indicates infection sometime in the past. Antibodies to EBNA develop 6 to 8 weeks after primary infection and are detectable for life.
What tube would be drawn if a physician has requested a Heterophile antibody screen?
Specimen Required Serum separator tube, lavender (EDTA), or pink (K2EDTA).
What is the common name of the infection caused by EBV?
Epstein-Barr virus, or EBV, is one of the most common human viruses in the world. It spreads primarily through saliva. EBV can cause infectious mononucleosis, also called mono, and other illnesses.
What are antibodies simple?
Listen to pronunciation. (AN-tee-BAH-dee) A protein made by plasma cells (a type of white blood cell) in response to an antigen (a substance that causes the body to make a specific immune response). Each antibody can bind to only one specific antigen.
What do antibodies do?
Antibodies are specialized proteins that are part of your immune system. They help protect against viruses, bacteria and other foreign substances. In the case of COVID-19, after you’re infected with the SARS-CoV-2 virus, your immune system recognizes the virus as a foreign substance and forms antibodies against it.
Are antibodies produced by plasma cells?
plasma cell, short-lived antibody-producing cell derived from a type of leukocyte (white blood cell) called a B cell. Each plasma cell can secrete several thousand molecules of antibody, thus releasing a large amount of antibody into the circulation. …
Why is latex agglutination testing commonly used?
Latex agglutination testing, also called latex fixation, is a diagnostic study that is widely used as a laboratory method to identify certain antibodies and antigens. The test uses a variety of body fluids including blood, urine, saliva and cerebrospinal fluid, which are dependable on what type of sample is needed.
What does C and T mean on a mono test?
Therefore, the presence of two colored bands, one at the Test position (T) and the other at the Control position (C), indicates a positive result, while the absence of a colored band at the Test position (T) indicates a negative result.
Is EBV glandular fever?
Glandular fever is caused by the Epstein-Barr virus (EBV). This virus is found in the saliva of infected people and can be spread through: kissing – glandular fever is often referred to as the “kissing disease”
What cells synthesize antibodies?
There are two main types lymphocytes: T cells and B cells. B cells produce antibody molecules that can latch on and destroy invading viruses or bacteria.
What is the principle of direct antigen testing?
The principle of DAT is to detect the presence of antibodies attached directly to the RBCs, which takes place by washing a collected blood sample in saline to isolate the patient’s RBCs; this procedure removes unbound antibodies that may otherwise confound the result.
Which antibody is elevated in acute infection?
1. Detection of IgM antibodies is often interpreted as an indicator of acute infection.
What is the meaning of Heterophilic?
[het″er-o-fil´ik] 1. having affinity for other antigens or antibodies besides the one for which it is specific.
What antibody does the Monospot test detect?
Monospot test (heterophil test). This quick screening test detects a type of antibody (heterophil antibody) that forms during certain infections. A sample of blood is placed on a microscope slide and mixed with other substances. If heterophil antibodies are present, the blood clumps (agglutinates).
What is a microscopic agglutination test?
The microscopic agglutination test (MAT) is the gold standard for sero-diagnosis of leptospirosis because of its unsurpassed diagnostic specificity. It uses panels of live leptospires, ideally recent isolates, representing the circulating serovars from the area where the patient became infected.
What are atypical lymphocytes in EBV?
These atypical lymphocytes (ie, Downey cells) actually are CD8 cytotoxic T cells. B-cell infection caused by EBV leads to the transformation of the B cells to immortal plasmacytoid cells, which secrete a wide variety of immunoglobulins (eg, heterophile antibodies).