.
Keeping this in consideration, how long does a person live after being diagnosed with cardiomyopathy?
A 2016 study estimated that about half of people who develop heart failure live beyond 5 years after being diagnosed. However, there is no simple answer for life expectancy rates, as the average life expectancy for each stage of CHF varies greatly.
Subsequently, question is, does cardiomyopathy go away? People who have cardiomyopathy but no signs or symptoms may not need treatment. Sometimes, dilated cardiomyopathy that comes on suddenly may even go away on its own. Treatment hinges on a few factors: the type of cardiomyopathy, the severity of your symptoms and complications as well as your age and overall health.
Subsequently, one may also ask, what is the mortality rate of cardiomyopathy?
Prognosis of Cardiomyopathy Fifty percent of patients die within 2 years; 25% of patients survive longer than 5 years. The two most common causes of death are progressive cardiac failure and arrythmia. The overall annual mortality from sudden death is 3-5% in adults and at least 6% in children and young adults.
How dangerous is cardiomyopathy?
As many as 1 in 500 adults may have cardiomyopathy, and many do not even know they have the condition. Cardiomyopathy is a leading cause of heart failure and the most common reason for needing a heart transplant. Cardiomyopathy is so dangerous because it often goes unrecognized and untreated.
Related Question AnswersIs cardiomyopathy a terminal illness?
However, patients with end stage disease can still be highly symptomatic. Over the last 10 years, there has been a realisation that heart failure (itself the final common pathway of several aetiologies such as hypertension, ischaemic and valvular heart disease, and cardiomyopathy) is a terminal illness.Can a heart function at 30 percent?
"When the ejection fraction gets down to less than 30 to 35 percent, the risk of cardiac arrest increases substantially," says Mitchell Faddis, MD, PhD, chief of electrophysiology at Barnes-Jewish & Washington University. Keep in mind that a healthy heart does not pump 100 percent of the blood out during each beat.Does cardiomyopathy qualify for disability?
Several types of cardiomyopathy can be eligible for Social Security disability benefits. Cardiomyopathy means any disease of the heart muscle. Depending on the type of cardiomyopathy, it can cause an enlarged heart or a weakened heart that cannot fill properly or pump blood properly.Can a blood test detect cardiomyopathy?
Diagnostic tests Your doctor may recommend one or more of the following tests to diagnose cardiomyopathy: Blood tests: A small amount of blood is taken usually drawn from a vein in your arm using a needle.Will enlarged heart go back normal?
Enlarged heart, depending on the cause may return to normal size if appropriate and timely treatment is given. In many cases it will not however, in which case the goal is prompt recognition and treatment to stabilize the situation and prevent further enlargement.Does cardiomyopathy show on ECG?
Electrocardiogram (EKG or ECG): An EKG records the heart's electrical activity, showing how fast the heart is beating and whether its rhythm is steady or irregular. An EKG can be used to detect cardiomyopathy as well as other problems, including heart attacks, arrhythmias (irregular heartbeats) and heart failure.Can you live 20 years heart failure?
Life expectancy with congestive heart failure varies depending on the severity of the condition, genetics, age, and other factors. According to the Centers for Disease Control and Prevention (CDC), around one-half of all people diagnosed with congestive heart failure will survive beyond five years.Can you exercise with cardiomyopathy?
Intensive or competitive exercise is not recommended for anyone with cardiomyopathy. Arrhythmic cardiomyopathy (or arrhythmogenic right ventricular cardiomyopathy or ARVC) - some types of exercise make this condition worse, and can increase arrhythmias and symptoms of heart failure in some people.What are the stages of cardiomyopathy?
Signs and symptoms of cardiomyopathy include:- Shortness of breath or trouble breathing, especially with physical exertion.
- Fatigue.
- Swelling in the ankles, feet, legs, abdomen and veins in the neck.
- Dizziness.
- Lightheadedness.
- Fainting during physical activity.
- Arrhythmias (irregular heartbeats)
Will a pacemaker help cardiomyopathy?
Cardiac resynchronization improves the symptoms of cardiomyopathy. Patients who have a delayed EKG are candidates for a biventricular pacemaker. Biventricular pacemakers help the heart resynchronize itself. You are able to treat the cardiomyopathy in conjunction with adequate medical therapy.How is cardiomyopathy diagnosed?
Your doctor may recommend one or more of the following tests to diagnose cardiomyopathy.- Blood Tests. During a blood test, a small amount of blood is taken from your body.
- Chest X Ray.
- EKG (Electrocardiogram)
- Holter and Event Monitors.
- Echocardiography.
- Stress Test.
- Cardiac Catheterization.
- Coronary Angiography.
Is viral cardiomyopathy hereditary?
Most viral infections don't cause heart problems, but occasionally a viral infection can affect the heart, causing cardiomyopathy. Hereditary factors. Some types of cardiomyopathy are inherited and affect several members of the same family. Coronary heart disease.Does cardiomyopathy mean heart failure?
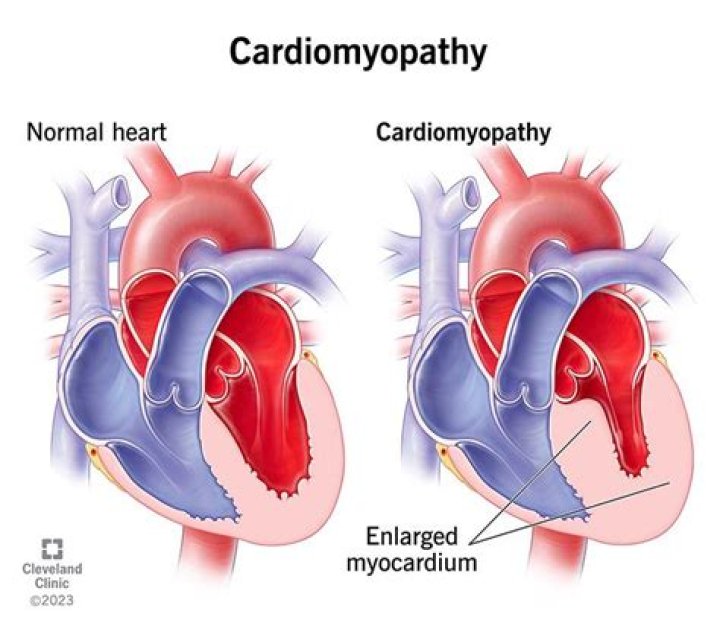
Cardiomyopathy (kahr-dee-o-my-OP-uh-thee) is a disease of the heart muscle that makes it harder for your heart to pump blood to the rest of your body. Cardiomyopathy can lead to heart failure. The main types of cardiomyopathy include dilated, hypertrophic and restrictive cardiomyopathy.Is restrictive cardiomyopathy fatal?
Outlook (Prognosis) People with restrictive cardiomyopathy may be heart transplant candidates. The outlook depends on the cause of the condition, but it is usually poor. Survival after diagnosis may exceed 10 years.Does cardiomyopathy cause chest pain?
Chest pain and shortness of breath often happen when you exercise. Over time, heart failure may come when the heart muscle becomes very thickened, which makes the heart work harder to pump blood. Along with chest pain, this type of cardiomyopathy may cause dizziness, lightheadedness, fainting, and other symptoms.What causes cardiomyopathy in adults?
Contributing factors for acquired cardiomyopathy include:- Long-term high blood pressure.
- Heart tissue damage from a heart attack.
- Chronic rapid heart rate.
- Heart valve problems.
- Metabolic disorders, such as obesity, thyroid disease or diabetes.
Can cardiomyopathy cause death?
Ventricular tachycardia and ventricular fibrillation can cause sudden cardiac death. People with hypertrophic cardiomyopathy have an increased risk of sudden cardiac death, although such deaths are rare. Sudden cardiac death is estimated to occur in about 1 percent of people with HCM each year.What are 4 signs of cardiomyopathy?
Symptoms- Breathlessness with exertion or even at rest.
- Swelling of the legs, ankles and feet.
- Bloating of the abdomen due to fluid buildup.
- Cough while lying down.
- Fatigue.
- Heartbeats that feel rapid, pounding or fluttering.
- Chest discomfort or pressure.
- Dizziness, lightheadedness and fainting.