.
Also know, are standards of conduct the same for every Medicare Parts C and D sponsor?
Medicare Parts C and D plan Sponsors are not required to have a compliance program. At a minimum, an effective compliance program includes four core requirements.
Subsequently, question is, does an effective compliance program includes four core requirements? CMS requires an effective compliance program to include seven core requirements:
- Written Policies, Procedures, and Standards of Conduct.
- Compliance Officer, Compliance Committee, and High-Level Oversight.
- Effective Training and Education.
- Effective Lines of Communication.
- Well-Publicized Disciplinary Standards.
Subsequently, one may also ask, what are some of the laws governing Medicare Parts C and D?
Some of the laws governing Medicare Parts C and D Fraud, Waste, and Abuse (FWA) include the Health Insurance Portability and Accountability Act (HIPAA); the False Claims Act; the Anti-Kickback Statute; the List of Excluded Individuals and Entities (LEIE); and the Health Care Fraud Statute.
What issues should be reported to a compliance department?
These are examples of issues that should be reported to a Compliance Department: suspected Fraud, Waste, and Abuse (FWA); potential health privacy violation, and unethical behavior/employee misconduct.
Related Question AnswersWhat are the consequences of non compliance?
The consequences of non-compliance are not limited to statutory or legal penalties- the indirect costs to a company are often more significant. These include the inconvenience and cost of righting a mistake, damage to the company's reputation or credit rating, and even possible loss of contracts.What is policy of non retaliation?
Non-Retaliation (20.089) Introduction. The purpose of this policy is to comply with applicable federal, state and local laws prohibiting retaliation and to protect employees who make good faith reports of potential violations of laws, regulations or University policy.What is correcting non compliance?
CORRECTING NON-COMPLIANCE. PROTECTS ENROLLEES, AVOID RECURRENCE OF THE SAME NON-COMPLIANCE, AND PROMOTES EFFCIENCY. STANDARDS OF CONDUCT ARE THE SAME FOR EVERY MEDICARE PARTS C AND PART D SPONSOR. FALSE.What is general compliance?
In general, compliance means conforming to a rule, such as a specification, policy, standard or law. Regulatory compliance describes the goal that organizations aspire to achieve in their efforts to ensure that they are aware of and take steps to comply with relevant laws, policies, and regulations.Does correcting non compliance ensure bonuses for employees?
Correct Choice X Protects enrollees, avoids recurrence of the same non-compliance, and promotes efficiency Ensures bonuses for all employees Both A.What is an effective compliance program?
Establishing an effective Compliance and Ethics Program ("Program") has become a necessity to protect any highly regulated organization. At its core, an effective Program protects an organization by detecting and preventing improper conduct and promoting adherence to the organization's legal and ethical obligations.Are practices that are inconsistent with sound fiscal business or medical practices resulting in unnecessary costs and improper payment?
provider practices that are inconsistent with sound fiscal, business, or medical practices, and that result in an unnecessary cost to the Medical Assistance Program, or that result in reimbursement for services that are not medically necessary or that fail to meet professionally recognized standards for health care.”What is a Medicare Part C plan?
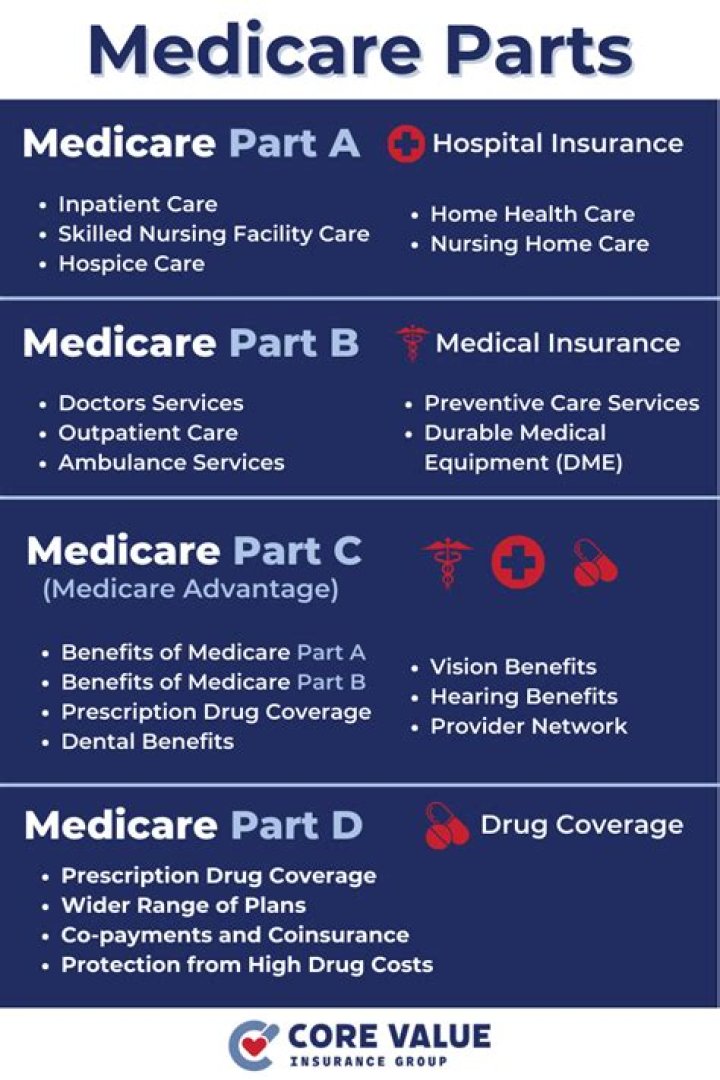
A Medicare Advantage Plan (like an HMO or PPO) is another Medicare health plan choice you may have as part of Medicare. Medicare Advantage Plans, sometimes called “Part C” or “MA Plans,” are offered by private companies approved by Medicare. Most include Medicare prescription drug coverage (Part D).What is Medicaid Integrity Program?
Medicaid Integrity Program - General Information. The MIP is the first comprehensive Federal strategy to prevent and reduce provider fraud, waste, and abuse in the $300 billion per year Medicaid program.What is waste in FWA?
Waste is overutilization of services or other practices that, directly or indirectly, result in unnecessary costs to the healthcare system, including the Medicare and Medicaid programs. It is not generally considered to be caused by criminally negligent actions, but by the misuse of resources.What are ways to report FWA?
How can I report fraud, waste, and abuse about an HHS program?- Toll-free phone: 1-800-HHS-TIPS (1-800-447-8477), 8:00 am - 5:30 pm, Eastern Time, Monday-Friday.
- Fax: 1-800-223-8164 (10 pages or less, please)
- TTY: 1-800-377-4950.
- Mail: HHS TIPS Hotline. P.O. Box 23489. Washington, DC 20026. (Note: please do not send any original documents)